Radio-Frequency Pain Management
Radio-frequency pain management treatment also known as ‘Radio-frequency Ablation’ is a relatively new and innovative option for patients who have experienced chronic or long term pain symptoms.
Most patients before this stage would have tried various other treatments to ease their symptoms such as holistic therapies which include acupuncture and massage, fitness and lifestyle changes and pain medication but would deem them to be unsuccessful in managing their pain. Some patients may have also received nerve block injections which were successful and hence is why they have been referred for radio frequency treatment.
What is Radio-frequency Ablation?
Radio- frequency waves are transmitted to heat a targeted nerve area to ablate them, essentially eliminating the transmission of pain signals to the brain.
Radio frequency ablation’s aim is to destroy nerve fibres carrying pain signals to the brain whilst being minimally invasive to the patient. It can provide a long lasting relief for people who experience pain in the neck, lower back, and arthritic joints and can be a simple and quick procedure which allows for the patient to go home on the same day.
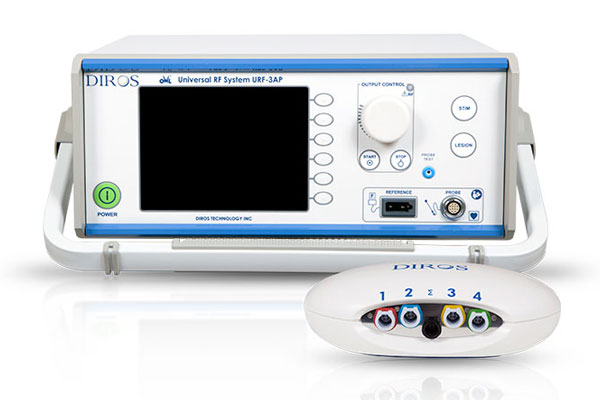
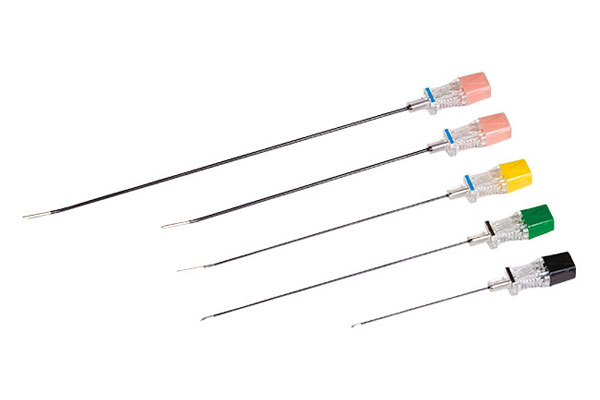
What to expect on Treatment Day
Stage 1
The patient lies on a table and is given a local anaesthetic to numb the treatment area. A low dose of sedative such as Versed or Valium may be issued to the patient at this point, however they will be fully awake and aware throughout the procedure.
Stage 2
With the aid of a fluoroscope, the doctor directs a thin hollow needle into the region responsible for the pain symptoms.
Stage 3
Once the needle is in place, a radio frequency current is transmitted through the hollow needle to the targeted nerve area to create a small lesion (approximately the size of a cotton swab tip).
Stage 4
The current destroys the part of the nerve that transmits pain and disrupts the pain-producing signal. After treatment the patient is monitored for a short period of time and then discharged. All in all the procedure can last anywhere between 15-45 minutes.
What are the Benefits of Radio-Frequency Pain Management?
The main benefit of radio-frequency pain management treatment is that it offers immediate pain relief to the patient with a little to no recover time and can significantly improve the patients quality of life without the need for surgery.
Other benefits include decreased need for pain medication, improved functioning and a quicker return to work and other physical activities.