What is Chronic Pain?
At a fundamental level, chronic pain is simply a matter of biology. It is caused by a bombardment of the central nervous system sending nociceptive pulses to the brain which then cause a change in the neural response.
There are many different factors to the cause of chronic pain, often conditions that accompany normal ageing may affect joints and bones in ways that cause pain symptoms. Other common causes can be injuries that fail to heal properly or nerve damage.
The most common form of chronic pain which people struggle to cope with is pain in the upper or lower back region which may be caused by a single factor or a combination of any of the following:
- Traumatic Injury
- Poor Posture
- Ageing of the Spine
- Congenital Spinal Conditions
- Lifting or carrying heavy objects
What treatments are available?
Chronic Pain is a complex condition that affects approximately two fifths of the UK population so treatment for each will differ.
Under the general category of medications there are both topical and oral therapies which can help manage the symptoms of chronic pain. Oral medications often include anti-inflammatory drugs or Opiods and others are medications that can be applied directly to the skin such as an ointment, patch or cream.
There are a number of other methods that may help with chronic pain which don’t involve medication. These things include:
- Regular Exercise
- Acupuncture
- Massage
- TENS Machine
- Drug-free Gels
These therapies may help relieve some of the pain and reduce the medication required to control it, giving a better quality of life to the patient.
Finally there are minimally invasive interventional techniques which can be used to help with the symptoms. These therapies are often recommended after the patient has trialled medication and non-invasive methods. Trigger Point Injections are one of the most common interventional techniques offered which involves injecting anasthetic and steroid into the area in and around the painful muscles and tissue.
In cases where all of the above treatments have been applied with little to no effect, a new and innovative treatment called Neuromodulation can be used as a treatment option.
Neuromodulation Spinal Cord Stimulation is a more long-term solution to pain management however it does involve a slightly more invasive procedure when compared to the trigger point injections. It involves a minimally invasive surgical procedure to insert a small device into the body which sends electrical signals to the spine, these currents then blocks the nerve activity to the brain, reducing the patients sensation of pain. The main benefits of Spinal Cord Stimulation therapy are:
Fast Recovery Rate – With some patients having experienced an almost instant recovery
Non Invasive Treatment – Quick turnaround, patients are often in and out on the same day
Accurately targets to specific areas – It will only target the areas receiving the pain signals.
 Chronic Pain Diagnosis
Chronic Pain Diagnosis
Pain is a very personal and subjective experience and unfortunately there is no test that can be used to measure and locate the pain with 100% precision. So, healthcare professionals rely on the patient’s own description of the timing, type and location of the pain. Defining whether it is dull, sharp, on-and-off or a constant type of pain to give the best clues as to the cause.
It is always best to speak with your doctor or a health care professional if you are experiencing symptoms of chronic pain since it may occur in a variety of locations within the body, patients and their health professionals must work together to identify the causes and symptoms so that a plan of adequate treatment can be arranged.
Chronic Pain Relief
It is always recommended that you speak to your healthcare professional about the treatments available to you however at Polar Medical we can supply a variety of Neuromodulation Products to help patients with chronic pain which include:
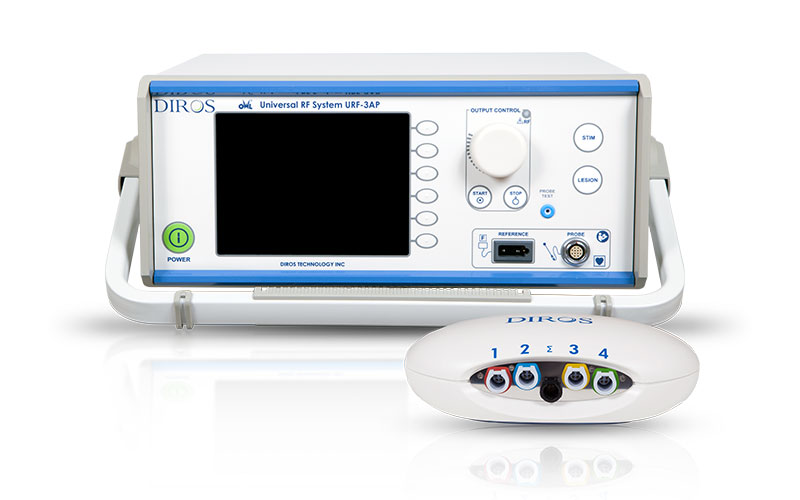
Diros Owl RF
Radio-frequency lesion generator targeting painful nerves.

